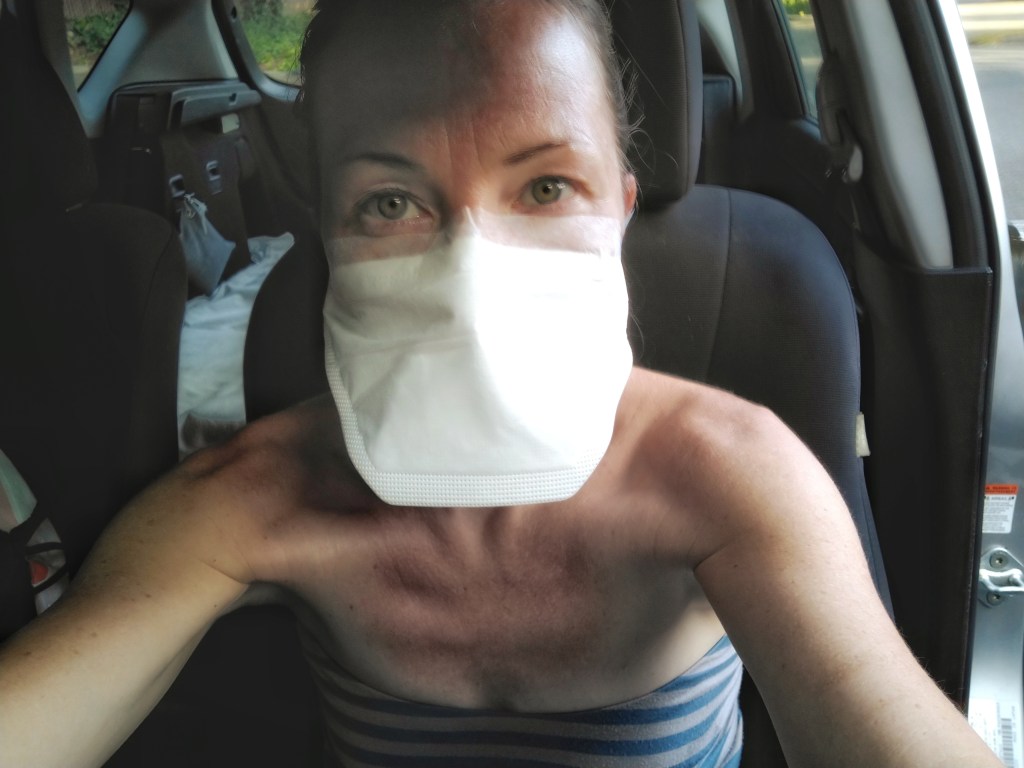
I’m going to start with the last things first:
In the next month, I am having a colonoscopy under anesthesia, a fluoroscopic barium defecography, an anorectal manometry, an ACTH (Cortrosyn) stimulation test, a transvaginal ultrasound, a thoracic MRI, skin prick allergy testing, a teeth cleaning and exam, an eye exam, and two blood draws. As well as trying to do IVIG every week and regular online doctors’ appointments.
What I really want to do is cancel everything, drive to the desert and live in peace.
The one thing I know for sure is that the more I rock this body’s boat, the worse things get, so I usually freeze and do nothing. But, lately, there seems to be a new mini-crisis most days, even though I took a long break from everything during the Omicron spike. It was lovely and peaceful for a while, but my body has been scaring me this month.
One day last week, my legs started to shake and then just buckled with no warning and I couldn’t walk. I had been moving a side table, so I guess I injured something, but I didn’t feel an injury, I just suddenly couldn’t walk and it is always in the back of my mind that I have a tethered spinal cord and leg/gait issues may get worse (many symptoms — like nerve pain — that could be attributed to tethered cord have gotten better, so I’m not convinced that “detethering” surgery is the answer for me).
Over the following days, unusual deep pain traveled from my buttocks to the back of my thighs to my left calf and then disappeared. During that time, I became desperate for a house with no stairs. I bought a bedside commode. I gave up a foster dog with whom I’d already fallen in love. Losing the limited mobility I have is terrifying. My husband would have to manage so much more and my quality of life would quickly plummet considering the energy it takes to keep my intestines working and food moving through. Not to mention losing dog joy, which is almost all joy in my world.
This week has been awful whack-a-crisis every day. Over the weekend, I was hit with terrible vertigo. This is one of the most sickening feelings — like your eyes are tumbling around in their orbits and you have to keep very, very still to stop from groaning outloud. It got mostly better the next day, but I still feel like I’m walking on a ship.
Monday, I had a pelvic spasm or bowel cramp so painful, I thought it was going to trigger a vasovagal collapse because I started to tremble and got weak and breathless.
Tuesday, I spent the day on the dog bed in front of the fireplace in a 76 degree room, shaking, chilled to the bone, with blood pressure all over the place, trying not to black out. I thought I’d left these episodes behind.
Yesterday, I developed an extremely bad right-sided migraine, which woke me out of sleep, panting from the pain and dreaming of IV narcotics — which I’m allergic to, but the pain was bad enough that I thought it wouldn’t matter if I stopped breathing, I’d let them inject anything to take the pain away.
So — it’s like that. In 14 days, I’ve gone on 3 scooter walks with Penny and I’m going out of my mind, desperate to get my slow, predictable days back.
In the midst of all this, I tried to continue weekly IVIG, which is undoubtedly the cause of some of this. I don’t know why it has turned on me and I don’t have words to describe the despair if I lose the one treatment that has helped me so profoundly.
I also saw another pelvic floor surgeon who was so rough while fitting me with a pessary, that I cried out involuntarily in her office. Her exam wasn’t even that bad in the grand scheme of things, but I was mute on the drive home, feeling traumatized by the brusque anal/vaginal invasiveness of it all. I only managed to keep that torture device inside me for 3 days because it made urinating very difficult. $100 down the drain and the only reason I was able to remove it was because I joined a FB pessary support group to get tips. Thank dog for other patients!
My biggest fear at the moment is the looming colonoscopy. I’ve been rescheduling it for 7 years. Before covid, I was cancelling out of fear — feeling the information gleaned from this test was outweighed by the risks. Just in the last 2 years, I’ve cancelled 8 times. They were legitimate reasons — covid spikes and my body being too unstable — but my GI doctor is frustrated and I still don’t feel confident that this is the right decision, even though it’s now 4 days away. My blood pressure is chronically low. I can’t get it to budge above around 85/55 — often lower. I wanted to try Fludrocortisone (a corticosteroid that can boost blood volume by increasing sodium in the body) before doing this procedure, but it takes me an excruciatingly long time to first get the nerve to try new medications, then to find a good day when I feel stable enough and then it takes weeks of eating little slivers to work up to a meaningful dose. It didn’t happen, along with dozens of other meds in my cupboard, waiting to be opened.

I was going to give myself IV fluids at home during the colonoscopy clean-out (I do my own peripheral IVs), but, in the last year, I’ve been having scary episodes and just this week realised they might be from IV saline. My vision starts to darken, like I’m going to black out, I get very cold and shake badly, my blood pressure spikes — this can go on for hours. It’s always the day after IVIG, so I stopped my infusions for 3 months, but then it happened when I did IV fluids without IVIG. I thought it must be the saline coupled with Midodrine, the low blood pressure medication I was on, so I stopped taking Midodrine and for 6 weeks, I was sure that was the answer. Until this week when it happened again.
My blood pressure has been dropping very low during IVIG, so, on top of the liter of IV saline, I’ve been drinking around 3 liters of salt/electrolyte water on infusion days (and eating a ton of salty snacks). It didn’t help boost my BP during the infusion, but I had another one of those episodes the day after. It almost feels like volume overload because my eyes get swollen, my BP spikes and I feel breathless, but my “high” blood pressure is still low by other people’s standards. During this episode the other day it was spiking to 107/74. How do you explain to a doctor that you’re in a “hypertensive” crisis when your BP is still lower than normal?

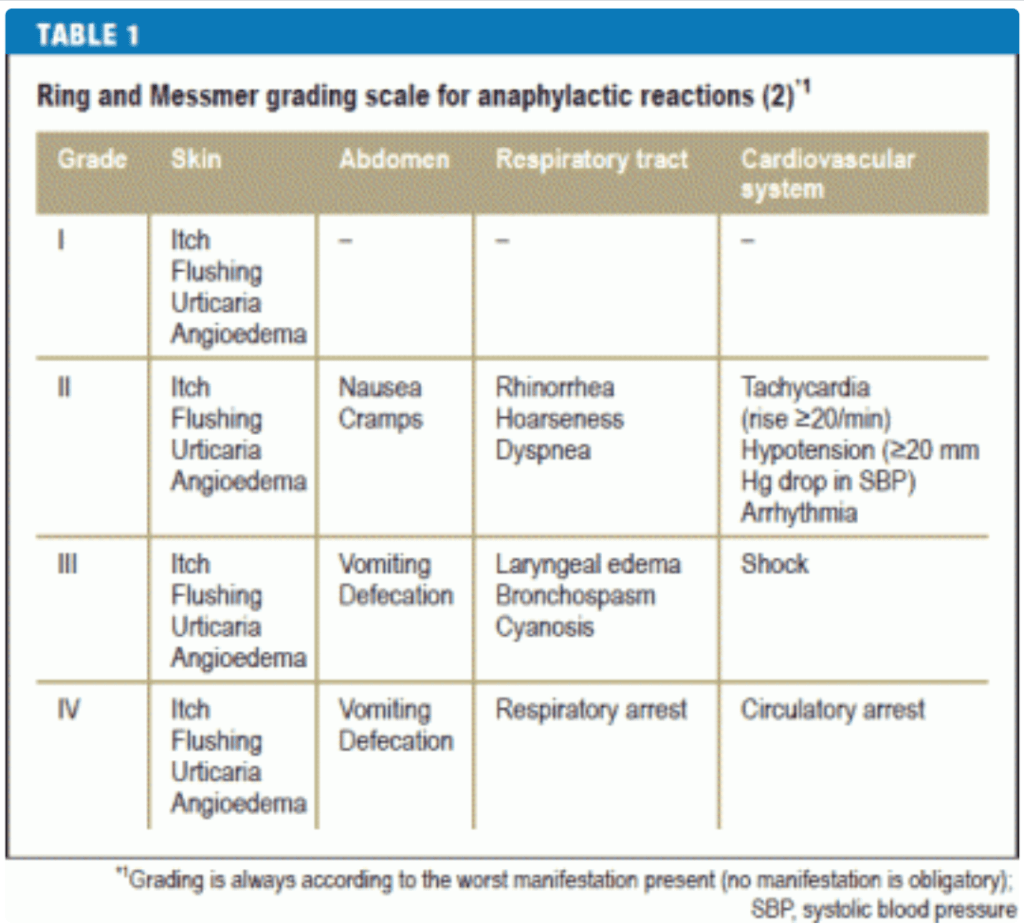
So, I’m about to start a dehydrating colon cleanout when I’m already weak from chronic hypotension, hemodynamically unstable, battling presyncope, having pelvic floor spasms and bowel pain, prone to hypoglycemia, my heart is tripping all over the place, and my brain feels like it’s going to explode out of my right eye. If I get through the prep without having to call the paramedics, I’m then meant to volunteer to let a stranger inject powerful sedatives and painkillers into my vein and hope that I don’t go into anaphylaxis or have my vitals bottom out. Or catch covid, for that matter, since vaccination is too risky, yet I have a primary immune deficiency, which feels like the worst combination during a pandemic.
Being released from the hospital and coming home almost feels the most reckless because all hell breaks loose in my body AFTER the fact. It’s in the middle of the night or the day after that the adrenaline wears off and the real problems start. I wish they’d admit me afterwards for observation, honestly, but it would be ludicrous to even ask. These are routine procedures that everyone gets done, after all.
But it doesn’t feel worth it. It feels dangerous. Which is part of why I’m writing this, I guess. I got out my advanced directive and durable POA. FFS.
We also found out this week that my healthy rock of a husband has a brain aneurysm and will need surgery. Surprise! That’s a story for a different time. But, really, forget all of my stuff. If anyone out there is going to send good thoughts/juju/prayers this way, please send them directly at my husband’s brain.