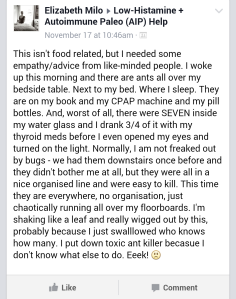
After 13 months of buildup, I’m finally scheduled for my first IgG infusion. Dr. Chia recommended I get IVIG (intravenous immunoglobulin) in August, 2014. When I came back to Seattle, I asked my GP about it and she said my total IgG wasn’t low enough (allopathic guidelines say total IgG < 400mg/dL) to warrant therapy. I asked my rheumatologist about it and he said because I have no evidence of persistent infections, I’d have to get an antibody vaccine provocation. I’m sure there’s a name for this, but, essentially, you are given a vaccine and then they look for an appropriate rise in antibody titers to that vaccine. If your body doesn’t mount a response, they can approve IVIG. Well, of course, I’m never getting a vaccination again, so that’s out of the question. I asked my main ND, Dr. W, and she said she didn’t have the ability to order it, but suggested oral IgG, which I never started because… another supplement, ugh. So, I’d given up on it when I went to a new ND, Dr. I, and I didn’t even think to mention it. After reviewing all my labs, the first thing she recommended was IVIG and, just like that, she got it approved. But… not so fast. That was 10 months ago and there was a lot of work to be done.
(As an aside, I do wonder if I’ve had low immunoglobulins my whole life and nobody looked into it. Or maybe it waxed and waned. I had chronic bronchitis, pneumonia and asthma as a child and, as an adult, got a chest infection pretty much once a year–probably more when I was smoking–but never thought this was unusual. Here’s a short article about one girl’s SCIG from infancy. It has some photos of infusions.)
Before trying IVIG, we decided I should try SCIG (sub-cutaneous IgG) because there are fewer side effects for most people. Before SCIG, I needed to test out the medications necessary to stave off anaphylaxis, aseptic meningitis, migraines and a host of other issues that can develop. Before testing the pre-meds, I had to make sure I could handle IV saline infusions since the last one I had caused a leaky anaphylactoid reaction. Before trying IV fluids, she wanted me to be on bioidentical progesterone, pregnenolone and DHEA, not only because my hormones are low, but also because there is evidence that hormone therapy can calm reactivity. And all of this has to be danced around my menstrual cycle because I’m somewhat reactive during ovulation and extremely reactive during my period. We also had to wait for me to get my nerve up because so much of this is dependent on my comfort level and, when anaphylaxis could be involved, I’m never comfortable.
I have friends in mast cell groups who “anaphylax” often, repeatedly, sometimes daily. I can’t imagine this. There are different levels of anaphylaxis, so I suppose these could be lower level reactions, but my episodes of anaphylaxis were full-blown and very scary, mostly because of the difficulty breathing. I really thought I would die and I probably have some PTSD from those experiences. No amount of sickness scares me as much as having a sudden anaphylactic reaction that kills me. I don’t want to get meningitis or be saddled with chronic migraines like my friend Jackie, but those are not at the top of my list of fears.
Having said that, I pay attention to comments like this since I, too, once had a CSF leak from a lumbar puncture and it was the 10 on my pain scale to which I now compare everything else. IVIG can mess you up:
(FYI, I found this website with tons of allergy information and graphics that might be interesting.)
So, I’ve been on topical, compounded hormones for almost a year and they haven’t raised my serum levels much, but I think they’ve helped with sleep (they also cause greasy skin and hair, like I’m going through puberty, but I’m willing to put up with that). At the beginning of this year, I was reeling from the terrible nocturnal reactions and tongue swelling I had been having, so I wasn’t willing to try anything new. Finally, in May, I got around to testing a tiny bag of IV saline (it went fine, although the whole appointment and clinic visit was a total shitshow which lead me to write two long emails to my doctor. I came very close to not going back, but I really want this treatment). Then in July, I had a full liter infused over 6 hours (a very long time for 2 bags of saline). Everything went fine, no problems (but no boost in blood pressure or energy, either), which meant it was time to schedule SCIG, but, once I started researching in earnest, I realised that there were so many questions I needed answered.
IVIG is often done in a hospital setting if the person is high-risk. I would prefer to have more than just a nurse present if I went into shock (and, by all accounts, nurses’ competency levels are highly variable). My doctor didn’t know how to get this done because the company with which she works does home infusions; she recommended I ask one of my MDs for help. More time ticked by while I emailed my GP (who has only met me once), my endocrinologist and my rheumatologist (both of whom have only met me a few times) for help with this. They all said no. I talked to the infusion company (who have been incredibly helpful thus far) and they offered to do it in their “infusion suite”, but there are no doctors present and their protocol is to call 911 if there is an emergency. Well, I live a few minutes from a fire house and an emergency room, so home seems just as safe as the infusion suite, if not more so since my husband, who is far-too-intimately acquainted with my history, can be there.
Scrolling through Facebook groups, I realise I have to learn how many injection sites I’ll have and whether to use my belly or thighs and the needle size and how many ml you can put in any one area and leakage, hardness, weals etc. etc. My good friend, who is braving his way through gruelling IVIG treatment, has been giving me advice every step of the way, which is invaluable when your doctor doesn’t tell you exactly what the process is or the importance of hydrating or the effects of IgA.
Different brands of IgG have varying amounts of IgA in them. In general, lower IgA equals fewer reactions and, if blood tests show that you have very low IgA or anti-IgA antibodies, you will qualify for the IgA-depleted IgG brands. Isn’t this something my doctor should have mentioned? She wrote the prescription for Gamunex and I asked her if she would consider Gammagard or Hyqvia, both of which have lower IgA. but she said it wasn’t necessary. And she may be right, but wouldn’t you want to use every tool available to keep your highly-reactive patient as safe as possible? My IgA has been slightly low in the past, so, right before I was meant to schedule my first infusion, I asked my doctor, “Can you test me to see if I have anti-IgA antibodies?” and she said yes. Doesn’t this seem like something that should have been done originally without my asking, considering my history?? Maddening.
The IgA test was meant to take a week to come back and I didn’t get the results for 3 weeks, so here we are in September. One of the IgA subclasses was low out of range, but I didn’t have anti-IgA antibodies, so I couldn’t really make a case for changing from Gamunex. And I wanted to do it as soon as possible rather than wait until after my next period, which would put us in October, so I scheduled it for this coming Tuesday.
My doctor wants me to take 2 Tylenol (Paracetamol), 2 Benadryl and 3mg of Prednisone (Prednisolone) before my treatment. I needed to test these premeds because last year when I took Prednisone, I worked up very slowly to 3mg, I only ever take 1 Tylenol at a time and I have been VERY sensitive to Benadryl since having M.E.–plus I’ve never taken the combo. I realised my EpiPens were expired and so were my two boxes of Benadryl and my emergency Prednisone. It took more waiting time for new prescriptions to be called in and finding a good day for my husband to pick them up. When he did, I realised they had given me 10mg pills of Prednisone rather than 1mg (always carefully inspect your pills!) and he had to go back to the pharmacy for a fourth time in a week. Poor guy.
Last week I tried 1 Tylenol, 1 Benadryl and 1.5mg of Prednisone (using my expired stash). About half an hour later, I got a tight chest. Not enough to scare me, but enough to put me off trying more Benadryl. Then I got very shaky and drowsy and had low blood pressure. After I slept for about an hour, I was incredibly thirsty and hungry and then, about 4 hours after taking them, I felt better than I have in a while and was chatty and good-humoured. Success.
Last night I tried again, this time with 2 Tylenol, 1 Benadryl and 3mg of (fresh) Prednisone. I couldn’t bring myself to take 2 Benadryl. The good news is, I didn’t get the tight chest and shakes this time, I just fell asleep for an hour. The bad news is, I didn’t feel good afterwards at all. I had a headache, my eyes and lips felt swollen, I was completely parched and felt really out of it and hungover. But, this is HUGE for me. It is so incredibly exciting to take a bunch of medications and come out unscathed. I’ve been wanting to test this for ages so I have some confidence that, if I’m given IV Benadryl and/or steroids in the event of an emergency, I’ll be okay.
A few final hurdles: I’m scrambling to get two blood draws on Monday before starting SCIG. Dr. W has been trying to get me to do regular “hydrotherapy” for a year and a half. It’s basically hot and cold towels over my torso and back, coupled with electrical stimulation (instructions for doing it at home can be found here). I never wanted to expend the energy until she told me about a patient of hers with hypogammaglobulinemia whose IgG levels came into the normal range after 6 weeks of hydro constitutionals. She was willing to test my total IgG before and after if I did this experiment. I love quantifiable evidence! So I started in August and, even though it’s only been 5 weeks, I want to get my levels tested again before starting SCIG.
The second thing is a babesia test. I’ve been asking my ND about this since June–in person during appointments, in email to her and also to her assistant, who keeps saying she has to get the doctor to sign the form–and can’t seem to get anywhere. They say yes, but it never happens. How hard could it be to sign a requisition form?? Her last message to me said I could get my blood drawn if I make another follow-up appointment. Are you kidding me? That seems downright cruel when we’ve discussed this at my last 3 appointments and she only works two days a week. I talked to the director of Igenex, the lab that does the testing, and he said I should definitely get it done before SCIG, so I finally just ordered the test kit myself and I’m going to bring it to my other doctor, Dr. W, on Monday and beg her to do the blood draw along with the total IgG. I don’t understand why everything has to be such a battle. It’s exhausting and infuriating.
I’m trying to not be annoyed at the difficult communication with my SCIG doctor because, not only is she the only one getting me this treatment, but she was willing to start me at 1 gram the first week (unheard of), building up to 5 grams over 5 weeks. She was also willing to prescribe saline infusions along with the treatment. Only 500ml each time, but every little bit of hydration helps mitigate side effects. I’m deeply grateful to have someone willing to do that when an immunologist wouldn’t even have a conversation about it.
Wish me luck. I’m going to receive all the supplies by courier on Monday and then Tuesday afternoon a nurse will come over, start the drip and show me how to do the sub-cutaneous injections. I believe after that, I’m on my own. Or, maybe because I’m getting IV fluids each week, a nurse will have to come, I don’t know. I will take Zyrtec and hydrate like mad the days before and after… But, friends and family, I am very scared. Even though it’s SCIG and not IVIG and even though I’m starting at a laughably low dose, I’m still scared. I will eat fairly low-histamine in the next few days and do my breathing exercises and meditations before, during and after treatment, but still… I want this to be the beginning not the end. Are my affairs in order? Do you all know how much I love you? Remember: when I first got sick and thought I was dying, I wrote down directives and requests. Husband, remember: the notebook in my bedside table.
Now everyone knock on wood for me and spit over your shoulders. Toba toba.