[Written Sunday morning:] Every morning I get up and vow to write some of the things crawling around my head and gnawing at my brain and then every day disappears into other things: cooking, feeling like crap, interacting with friends in my facebook group, reading, researching, tv… Today, I’m sequestered in one room while the cleaning lady tackles the rest of the house and I want to do a wee catch up.
Two months after the horrific Cromolyn-induced crash, I’m feeling much better. Not as good as I was beforehand, but so much better than I anticipated I would. If it takes 3 or 4 months to get back to where I was, that will be great–much better than the years I thought it would take (or the never I feared might happen). When I got home from the AirBnB rentals, my husband had cleaned out my bedroom: no furniture besides the bed and bedside table, no more clothes or books, everything hoovered and wiped down with ammonia. He put a vapor barrier up at the top of the stairs–one of those plastic doorways used in construction sites or the house in the film E.T.–and the upstairs is strictly a dog-free zone. Oh, it breaks my heart not to be able to snuggle with my kids and it crushes me when they hear me moving around and whine at the gate we have across the stairs. Another downside is, I’m doing far fewer preemptive rests and meditations because I don’t want to leave them and go upstairs. It used to be our routine to head upstairs a few times a day and lie down. My Little Guy had the times programmed in his brain and would bark to come in from outside and look at me like, “Let’s go, Mama! You need to meditate.” That doesn’t happen anymore and my brain and body are feeling the effects. However, I will begrudgingly admit that it is really reassuring to know that I am spending 12 to 15 hours a day in minimal dander and dog hair. I wake up feeling cleaner internally. That has got to help my poor struggling body, so I’m very grateful for all the hard work my husband put into dedogifying the upstairs.
What it used to be like:

What I see now from the top of the stairs:

I haven’t been sleeping very well. Much better than when I was horribly sick, of course, but not as well as I was in the last two rentals. My sleep in that last rental was amazing– I would close my eyes at 11pm and open them at 7am. A few nights that I was there, I woke up after 8am! Never, ever, ever have I slept straight through for over 8 hours without waking up from crazy dreams or painful bones and muscles. It was glorious… besides the fact that I felt poisoned by the new Ikea wardrobes. I wonder if the off-gassing from the new furniture was somehow drugging me into a stupour? Also part of the problem is my apnea devices. I continue to avoid the CPAP because it wakes me up constantly, but the new oral appliance has its own issues. I got the Narval by Resmed, made by a 3D printer.
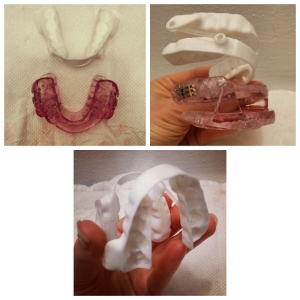
The white one is the bendy, light Narval. The pink one is the heavy, rigid nightmare I was trying to use before.
It is incredibly thin and light and bendy, which is everything I wanted and I’m able to fall asleep while wearing it… BUT. … I have worse TMJ issues than I realised and it causes so much pain. Every day, my jaw hurts, my temples ache, my head hurts and then, about once a week, I have a really rough, tense grinding night and I wake up feeling like my jaw is dislocated. It is painful to move and chew and clicks alarmingly. This can’t be good. So, I keep sleeping with no oral appliance or CPAP and I can definitely feel the difference in how I feel in the morning–less rested, more pain, but my jaw in tact. So, what am I to do?
I’ve started seeing my “physical therapist” again. Aka Magic Fingers. He is so wonderful for me. After a 3-month hiatus, the day I returned happened to be the day after he finished a course on strain-counterstrain for the nervous system. The teacher of whatever magic he does flew out to Seattle from the East Coast and trained a group of 30 practitioners. He said, “I’m one of only 30 in the world that have been trained to do this and you are the number one person I want to work on because your nervous system is a mess.” I keep my appointments with him no matter what. I even went last week when he was getting over a cold.
Speaking of colds, it has been 3 years and 19 weeks since I last had a cold. I’m amazed by that. I still live in fear of the day I catch a cold, especially since Dr. Chia said one virus could wipe me out and set back my recovery significantly, if not permanently. You may remember that he recommended I get IVIG to bolster my immune system and protect myself from all you sickies out there. Well, my MD referred me to University of Washington Immunology and they turned me down because my total IgG wasn’t low enough. So, I talked to my ND, Dr. W, and their clinic isn’t licensed to do it. On a whim, I went to see another ND, Dr. I, at a different clinic–mainly because they take insurance and I wanted to have a back-up doctor if I had to stop seeing Dr. W (who does not take insurance and, even with discounts for being unemployed, costs me too much money). The first thing Dr. I said when I came in was, “I think you need IgG.” Oh, bless her. There is hope for this treatment! But let me back up…
So, this new clinic requested all my test results in advance, they photocopied the entire binder and the doctor had reviewed it before I got there. They asked me to run my 23andMe results through MTHFRsupport.com and send them the results (so far, I’ve had 3 doctors tell me they know about methylation and nutrigenomics, but not a single one actually has addressed it. See some of my MTHFRsupport.com Genetic Variance Report here). The clinic has an IV infusion room, looking all dim and cozy, with plush recliners and blankets. They have a hyperbaric oxygen chamber! Something I have been curious about trying for over a year since I read Dr. Deckoff-Jones’s blog. And the clinic is 4 minutes from my house. Score. Dr. I ordered a load more tests and is willing to consider sub-cutaneous immunoglobulin first since I’m a scardy-cat about jumping right into IVIG (assuming we can get either of them approved by insurance, that is). A few days after our appointment, I went to the lab for a blood draw because she wanted to get updated tests and I see her again next week.

It’d be nice if they left some blood in my body.
Speaking of test results (which can all be found here), I never mentioned the hormone panel and blood test results ordered by Dr. W in the last few months [bold type is for my benefit, so I can access this info easily when I look back). My varicella zoster IgG, IgM and HSV IgM were all positive. All coxsackie A viruses were high and all coxsackie B except for 3 and 4 (although 4 was high in Dr. Chia’s tests). EBV IgG was high indicating a reactivated infection. My total IgG was even lower than when Dr. Chia tested and, as I mentioned before, my thyroid was tanked: TSH, T3 and T4 all low. But the hormone panel was slightly alarming: almost everything was low: DHEA, progesterone, testosterone, estrone, aldosterone, androsterone, pregnanediol, tetrahydrocortisol and on and on. Not sure how concerned I should be, but Dr. W put me on topical DHEA (about 5mg rubbed into my abdomen in the mornings) and supposedly that should help something. It’s been a month now and the only difference that I’ve noticed is my period was 3 weeks late after I started it. My period has pretty much been every 28-29 days for 25 years. I just descovered today that it has MSM in it, which I’m not meant to have because of my sulfur issue. I’ll ask her about it when I see her on Wednesday.
So here’s what I’m taking currently:
Topical DHEA
Probiotics
Riboflavin-5-phosphate
Trace Minerals
Vitamin C
Vitamin D3
Vitamin K2
Fish oil
1/3 of a capsule of B complex #6
Magnesium
Biotin sporadically
Zinc sporadically
Charcoal sporadically
Quercetin sporadically
Gentian/Wormwood sporadically
I also started oil pulling a few times a week (when I remember) against my better judgement, but my nutritionist thought I should give it a try, so, why not?
I try to use my dry skin brush about once a week.
I am in my third month of Restasis and my eyes are worse than ever. They are never not bothering me. Swollen, itchy, tingly, burning, blurry, gritty. Always.
I have a new pillow, which is a god-send for my bursitits in my shoulders, but I had to let it off-gas outside for over a month. It still slightly concerns me, so I emailed Dr. Bob and here’s what he said: “We do not use flame retardants or any other harmful chemicals. On the Amazon site you can see our product obtained the Oeko-Tex Standard 100 Certification. This is a difficult certification to receive and shows this testing lab certifies the pillow is free of harmful chemicals. Oeko is the best know lab and certification for products to be free of harmful chemicals.” Hmmm… well, this thing stinks and I hope it isn’t off-gassing into my brain.
I love love LOVE having short hair. Can’t believe I didn’t do it sooner. Hair is such a nightmare when you’re sick and the cut disguises all the hair loss in the front.

Grainy photo, but you get the gist.
What else?
I’m still on a modified AIP (autoimmune paleo) plus low-histamine-ish diet. I am not strict on AIP or low-histamine becasue I’m always trying to reintroduce foods back into my diet so I can have as many nutrients as possible and don’t develop even more sesntivities. I constantly warn everyone on my Facebook group not to take an elimination diet lightly and add back as many foods as possible as quickly as possible. It becomes a trap. Eating fewer foods causes a host of new issues (in my case, gastroparesis, worsening constipation and odd reactions that I never had before embarking on AIP). Also, the longer you don’t eat them, the harder they are to get back — both physically and mentally. Hence the reason I never eliminated ice cream, chocolate and packaged chips. God forbid I lose my unhealthy addictions. I need the soul food (although, I do really think one of these days I have to see if I feel better without sugar in my life. It’s just that it was easier to quit gluten, dairy, drinking alcohol and smoking than it seems to be to even contemplate eliminating sugar for a few weeks). One of these days I’ll write a post on what I eat on this diet, but, in the meantime, you can see photos on my Instagram account, if you’re interested (minus all the crap I eat–I’m trying to inspire people, after all, not cause them inflammation).
We ordered a free-range, organic, recently-harvested, fresh (not frozen) turkey for pick up today for Thanksgiving, but, to keep histamines low, we have to roast it right away (and then my husband freezes the leftover meat for me and makes bone broth from the carcass), so we are celebrating Thanksgiving today. We were going to have a get-together with our friends, Z and J, and my sister and her boyfriend (hence the cleaning lady), but it fell through, so the two of us are going to sit down to a 12-pound turkey alone. It’s ok. I’m thankful that I was feeling almost well enough to have some people over for the first time in 2.5 years. I’m thankful that I still have some people in my life to invite over. I’m thankful that I will have a yummy dinner and I don’t even mind that almost every meal I eat looks like Thanksgiving dinner and there really won’t be any different fun stuff. At least I’ll have turkey instead of chicken. And maybe the tryptophan will help me sleep!
Speaking of food, I’m starving and the cleaning lady is in the kitchen. I don’t want to get in her way or have to chat, so I’m trying to think of what else I can tell you all.
I made it to the freezing cold cemetery on the scooter for about 40 minutes a few weeks ago, wearing about 5 layers and carrying a hot water bottle. It was literally my first time spending some time outside in a month. The winter is hard that way. It really feels unhealthy to be trapped inside 24 hours a day. I have to make an effort to put on my coat and hat and go out into the garden. Please remind me!

We bought a proper comfy dog bed for the kids seeing as they are arthritic and bony (it was on sale, has no fire retardants and is returnable at any time, even if used). It’s the size of a small country. 110-pound Bowie is thrilled when he can actually lie in it and Little Guy doesn’t relegate him to the crappy small bed.


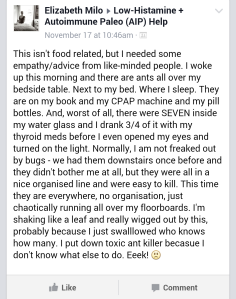
I found ants in my room one morning. They were running in droves all over the floor. It took days and days to kill them and there are still carcasses strewn about. It was pretty gross.

I’m still going to therapy. It’s been great recently. He’s very interested in cultural history as a jumping-off point and that is helpful for someone who mourns the loss of Ireland and regularly starts blubbering over how powerfully I miss it.
I have a lot of issues to work out there– An American by birth who never questioned that I was Irish, but wound up back in America and then felt rejected by the country I love… Marrying a man with an identical upbringing and thinking, “how perfect! We can relocate back home,” but it’s not home to him anymore… staying in America by default, year after year, but always wishing I was in Ireland and planning the eventual return… and then getting a disease that stops me from returning, so I have no choice, anyway. My therapist asked me if I’d be able to manage my illness better if I were living in Dublin and I said yes because my mother, aunt and best friend live there. And so does my heart. But it’s a difficult place to live and we’d have no money, so that’s not the answer.

Ok, I can’t avoid it any longer, I have to eat. And that was really dredging the bottle of the barrel for stuff to tell you about.
I’m thankful for all of you, too, dear readers. You have no idea. Love and thanks and nom nom nom gobble gobble to everyone this week. X














